 Trish discovered the newest lump in early March as we were doing our presentation at SXSW in Austin Texas. Sadly, and ironically, that presentation was on crowdsourcing cancer support and drew heavily on our last experience with cancer in 2010.
Trish discovered the newest lump in early March as we were doing our presentation at SXSW in Austin Texas. Sadly, and ironically, that presentation was on crowdsourcing cancer support and drew heavily on our last experience with cancer in 2010.
I flippantly dismissed the lump in her right neck-shoulder as an inflammation. But Trisha worried about it, and went to check it out when we got back. Dr. Carolyn Hendricks, her oncologist since 2003, immediately identified it as cancer but recommended more tests to be sure. (Note to self: Shut the fuck up. You don’t know anything. Thank you.)
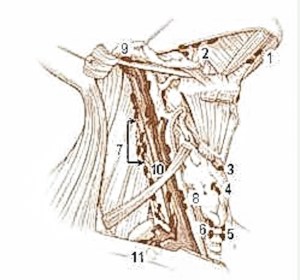 The tests showed she has breast cancer in her supraclavicular node, a group of a dozen lymph nodes at the bottom of a long lymphatic superhighway that runs along the neckline. It’s one of the major pathways for lymph in the body and is very common to become infected with any type of cancer. (#11 at bottom.) Supraclavicular nodes are sentinel, or warning nodes.
The tests showed she has breast cancer in her supraclavicular node, a group of a dozen lymph nodes at the bottom of a long lymphatic superhighway that runs along the neckline. It’s one of the major pathways for lymph in the body and is very common to become infected with any type of cancer. (#11 at bottom.) Supraclavicular nodes are sentinel, or warning nodes.
We waited an agonizing week for the results of the CaT and Bone scans, which blessedly came back negative. It wasn’t in her vital organs – a huge relief. And it could mean that this is a a new Stage II or III cancer of another type, which would give her more hope than a metastasis.
 But the biopsy revealed it was still triple negative breast cancer cancer, the same kind she had in her primary site on the other side. And because it has apparently moved across the body through the blood stream and infected a distant site, it is classified as a metastasis, stage IV.
But the biopsy revealed it was still triple negative breast cancer cancer, the same kind she had in her primary site on the other side. And because it has apparently moved across the body through the blood stream and infected a distant site, it is classified as a metastasis, stage IV.
But the diagnosis is slightly complicated. Typically, once a cancer gets loose in the bloodstream, it forms sites in multiple places. Trish has it in only one spot, her supraclavicular node, and it’s fairly big – 2.5 cm. It’s uncommon for it to be found in this way. This raises the slim possibility that this is actually a new stage III cancer from her right breast.
But the three oncologists we have talked to all agree it’s highly unlikely that this is the case, and are emphatic that we must treat this as if it is a Stage IV metastasis. They also all admit that this is an unusual and early stage IV cancer. There is a sliver of hope it might be different or more treatable than ‘typical’ stage IVs but we won’t know that for a long time.
 Trish and I are not unaccustomed to strange cancer diagnoses. Her second bout with cancer in 2010 was also a mystery because it reappeared in exactly the same site as the primary in 2004. But with 6 years in between occurrences, the doctors could not rule out that it was a new primary cancer – the oncological equivalent of being struck by lightning twice in the same place.
Trish and I are not unaccustomed to strange cancer diagnoses. Her second bout with cancer in 2010 was also a mystery because it reappeared in exactly the same site as the primary in 2004. But with 6 years in between occurrences, the doctors could not rule out that it was a new primary cancer – the oncological equivalent of being struck by lightning twice in the same place.
Stage IV is not considered curable because once the cancer figures out how to spread across the body, it’s difficult – statistically impossible – to eradicate. Trish’s cancer (assuming it’s been the same one all along, which is most likely) has survived two surgeries, FEC chemotherapy , TAC chemotherapy and 6,000 rads of radiation. It’s an aggressive one and it’s not going away easily.
 Stage IV is treatable, and Trish has caught this one early – so early that the oncologists want to do radiation on the lump, which is an unusual treatment for stage IV. By the time Stage IV cancer is loose in the body, it becomes pointless to do surgery or localized radiation anymore. Doctors focus their efforts on systemic treatments like chemotherapy.
Stage IV is treatable, and Trish has caught this one early – so early that the oncologists want to do radiation on the lump, which is an unusual treatment for stage IV. By the time Stage IV cancer is loose in the body, it becomes pointless to do surgery or localized radiation anymore. Doctors focus their efforts on systemic treatments like chemotherapy.
But since Trish’s has only appeared in one place, they are recommending 6,000 more rads of radiation on that lymph node. The radio-oncologist, a nice guy who sits uncomfortably close to you when he consults, cackled when he said ‘We’re gonna fry that node’. There was a little gleam in his eye too. If she kills the cancer in that node, and gets another clear body scan, she would be ‘in remission’ or NED (No Evidence of Disease) by early May.
 Trish asked three doctors about the viability of surgery to remove the node, and all said it was not advisable – each for different reasons. The oncologist cited statistical evidence that it would not help, the radiation doc said the radiation would do a better job of killing it and the surgeon said it would be too complicated given the location and number of infected nodes.
Trish asked three doctors about the viability of surgery to remove the node, and all said it was not advisable – each for different reasons. The oncologist cited statistical evidence that it would not help, the radiation doc said the radiation would do a better job of killing it and the surgeon said it would be too complicated given the location and number of infected nodes.
After the six weeks of radiation, Trish will most likely begin chemotherapy. It’s not strictly required, because she will (most likely) be in remission. Some people preserve their quality of life once they achieve remission. Having done two brutal chemo-therapies, Trish would know better than any of us how to make that call.
 But I think she is leaning toward starting prophylactic chemotherapy to be safe. The primary oncologist suggested Capecitebine, which is a pill form of chemo you can take daily. The side effects are considered to be milder although they include radical dryness of the hands and feet and diarrhea.
But I think she is leaning toward starting prophylactic chemotherapy to be safe. The primary oncologist suggested Capecitebine, which is a pill form of chemo you can take daily. The side effects are considered to be milder although they include radical dryness of the hands and feet and diarrhea.
Still, maintaining her energy to do dance, trapeze and travel is her most important quality-of-life goal right now, so a low-side-effect chemo makes good sense. Dr. Hendricks also offered a few experimental clinical trials but they would come with more severe side effects.
 She’ll get tested every 8-12 weeks with bone scans and CaT scans, and the appearance of breast cancer in her bone, lungs, liver or brain would signal the next level of disease progression. We would conclude at that point that the Capecitebine is no longer effective, and she would begin trying other Chemotherapies to contain the cancerous cells.
She’ll get tested every 8-12 weeks with bone scans and CaT scans, and the appearance of breast cancer in her bone, lungs, liver or brain would signal the next level of disease progression. We would conclude at that point that the Capecitebine is no longer effective, and she would begin trying other Chemotherapies to contain the cancerous cells.
It becomes a race against time at that stage and is something I can barely even think about. But we’ll cross that bridge with humor and courage when it becomes necessary.

Keep fighting!
Love, Dad